Hyperbaric Oxygen Therapy for Diabetic Ulcers
Associate Professor (ret’d) F Michael Davis, formerly Medical Director, Hyperbaric Medicine Unit, Christchurch Hospital
Summary
- Hyperbaric oxygen therapy (HBOT) improved healing in six prospective randomised trials (RCT) of diabetic ulcers and reduced the rate of major amputation in two.1–6 In an additional RCT of mixed aetiology leg ulcers, including diabetic ulcers, healing was improved with HBOT.7
- HBOT has been shown to be cost-effective even though it is a moderately expensive therapy.4
- After HBOT, healing is maintained in the medium to long term because vascular neogenesis is promoted.1,5,8
- Complication rates of HBOT are low and treatment is well tolerated by the majority of patients.
- HBOT must be used in conjunction with good multidisciplinary wound care.
What is hyperbaric oxygen therapy
Hyperbaric oxygen therapy
(HBOT) is the intermittent administration of 100% oxygen at pressures greater than normal ambient pressure. There are several ways to provide this, all of which require a pressure vessel in which the patient(s) sit or lie for 2–3 hours daily for several weeks.
The clinical evidence for HBOT
Six small, prospective randomised trials of HBOT for diabetic ulcers have been published.1–6 All show improved healing and, in two, a reduction in major amputation rate was reported (Table 1). Follow-up studies suggest these benefits are maintained in the medium to long term (3–5 years).8 However, a recent Cochrane review concluded there was a need for further large randomised studies because the trials (Table 1) had various flaws in design and/or reporting not meeting Cochrane criteria.9
HBOT is a moderately expensive treatment. In Christchurch, the estimated cost of a 30-treatment HBOT course is approximately $12,000 per patient. However, the cost-benefit studies from the UK and USA show an overall saving by combining HBOT with standard modalities of care in the management of diabetic ulcers, as well as improved outcomes.4,8 The UK study reported an overall saving of approximately NZ$8,000 per patient treated compared to non-HBOT care.4
Locally, we have too small a database yet to have a good idea of how well we are doing. However, of the first 50 lower limb ulcers of mixed aetiology (approx. half DM ulcers) referred to HMU, 18 (36%) were healed and 7 (14%) substantially improved on medium-term (approx. 3 month) follow-up (NNT for improvement = 2). There has been no major morbidity from HBOT in these patients. An on-going prospective cohort Australasian study of HBOT for problem wounds, both diabetic and non-diabetic, with over 400 cases shows a similar early post-HBOT healing rate, increasing to over 75% at one year, irrespective of the aetiology. Despite the Cochrane conclusions, we are firmly of the view, from our local clinical experience that HBOT, combined with multidisciplinary wound care improves healing in selected patients.
How HBOT works
There are diverse actions of HBOT, including support of oxygen-dependent healing processes and, more importantly, cell-signalling effects that accelerate these processes for many hours beyond the HBOT exposure. The intermittent restoration of steep oxygen diffusion gradients in the peri-wound area stimulates fibroblast function in a dose-dependent manner.10,11 The cyclical pattern of hyperoxygenation/hypoxia leads to the release of local humoral mechanisms promoting wound healing. Recent work suggests a positive effect on nitric oxide metabolism in the diabetic wound. These changes result in an advancing field of neovasculogenesis. At the same time, oedema is reduced improving perfusion, and macrophage function is enhanced, particularly the ‘oxygen burst’ phase, in the hypoxic diabetic wound. HBOT is known to work synergistically with several antibiotics. Daily HBOT also corrects deficient neutrophil adhesion in Type II diabetes.
Whom to refer to HBOT
Any diabetic patient in whom a wound is not healing after a reasonable period of multidisciplinary wound care should be considered for HBOT. The international consensus is that an ulcer failing to respond after six weeks (or earlier, if the ulcer is limb-threatening) and for which no correctable large vessel disease is present should be referred for assessment for HBOT. Renal failure and concomitant major arterial disease carry a poorer prognosis for healing with HBOT just as they do with other interventions. Anecdotally, HBOT has been reported to be particularly useful in the neuropathic and Charcot foot.
The evidence in non-diabetic ulcers is more limited than for diabetic ulcers, but the same broad principles apply and HBOT has been shown to enhance healing in one small, prospective, randomised study.7
Problem wounds secondary to accidental trauma or medical misadventure in both diabetic and non-diabetic patients may be referred for assessment for HBOT under a prior approval ACC contract that has been in place nationally since March 2002. Many potential referrers are still unaware of this ACC-funded service.
Referrals to the Hyperbaric Medicine Unit at Christchurch Hospital may be made directly from primary care.
HBOT facilities in New Zealand
There are clinical HBOT facilities in Christchurch and Auckland, at the RNZN Medical Centre and at Quay Park Medical Centre. The only hyperbaric facility in New Zealand based in a civilian, tertiary-referral hospital is at Christchurch Hospital.
Table 1. Summary of randomised studies of hyperbaric oxygen therapy in diabetic and non-diabetic ulcers
|
Study
|
Patients |
Outcome Measure |
Results |
Statistics |
Comments |
| Kalani et al1 |
38 |
Healed ulcer Amputation |
13/17
2/17
|
10/21
7/21
|
<0.05
<0.05
|
follow up 3yr |
| Faglia et al2 |
68 |
Amputation |
3/35 |
11/33 |
<0.02
|
|
| Doctor et al3 |
30 |
Amputation |
2/15 |
7/15 |
<0.05 |
weekly HBOT only |
| Abidia et al4 |
18 |
Healed ulcer at 1yr
Wound area decrease
|
5/8
100%
|
1/8
52%
|
0.026
0.027
|
saving approx $8000per patient |
| Hammarlund & Sundberg7 |
16 |
Wound area decrease at 6 weeks |
35.7% |
2.7% |
0.001 |
Diabetic and non-diabetic ulcers |
| Lee et al5 (abstract only) |
32 |
Wound healing time
Minor amptation
Mortality
|
not
4/20
not
|
stated
4/12
stated
|
0.03
0.005
0.03
|
HBOT group had severer wounds; 2yr follow up |
| Londahl et al 6 |
94 |
Healed ulcer at 1yr |
30/49 |
12/45 |
0.009 |
double blind |
| |
Amputation: BKA or AKA |
|
|
|
References
- Kalani M, Naderi N, Lind F, Brismar K. Hyperbaric oxygen therapy for wound healing and limb salvage in diabetic foot lesions: Three year follow-up. Undersea Hyperb Med 2000; 27(Suppl): 44-45
- Faglia E, Favales F, Ealdeghia et al. Adjunctive systemic hyperbaric oxygen therapy in treatment of severe prevalently ischaemic diabetic foot ulcer. Diabetes Care 1996; 19: 1338-1343
- Doctor N, Pandya S, Supe A. Hyperbaric oxygen therapy in diabetic feet. J Post Grad Med 1992; 38: 112-114
- Abidia A, Laden G, Kuhan G et al. The role of hyperbaric oxygen therapy in ischaemic diabetic lower extremity ulcers: A double-blind randomized-controlled trial. Eur J Endovasc Surg 2003; 25: 513-518
- Lee C-T, Ramiah R, Choong SK, Seng KC, Rajoo V. Adjunctive hyperbaric oxygen in diabetic foot ulcers: a randomized, prospective, double-blind study. Proceedings of the Undersea and Hyperbaric Medical Society Annual Scientific Meeting, Sydney, 2004.
- Londahl M, Katzman P, Nilsson A, Hammerlund C. Hyperbaric oxygen therapy facilitates healing of chronic foot ulcers in patients with diabetes. Diabetes Care. 2010;33:998-1003.
- Hammarlund C, Sundberg T. Hyperbaric oxygen reduced size of chronic leg ulcers: a randomized double-blind study. Plast Reconstr Surg 1994; 93: 829-834
- Cianci P, Hunt TK. Long term results of aggressive management of diabetic foot ulcers suggest significant cost effectiveness. Wound Rep Reg 1997; 5: 141-146
- Oriani G, Faglia E, Favales F, Quarantiello A, Calia P, Michael M. Hyperbaric oxygen (HBO) in the treatment of diabetic gangrene. Proceedings of XXIst Annual Meeting of EUBS on Diving and Hyperbaric Medicine, Helsinki, Eds. Sipinen SA, Leinio M 1995: 120
- Kranke P, Bennett M, Martyn-St James M, Schnabel A, Debus SE. Hyperbaric oxygen therapy for treating chronic wounds. Cochrane Database of Systematic Reviews 2012, Issue 4. Art. No.: CD004123. DOI: 10.1002/14651858.CD004123.pub3
- Hunt TK, Pai MP. The effect of varying ambient oxygen tensions on wound metabolism and collagen synthesis. Surg Gynecol Obstet 1972; 135: 561-567
- Hehenberger K, Brismar K, Lind F, Kratz G. Dose-dependent hyperbaric oxygen stimulation of human fibroblast proliferation. Wound Rep Reg 1997; 5: 147-150
Advice following a diving accident
The Christchurch Hyperbaric Medicine Unit provides a 24 hour acute service for NZ south of Taupo, on request from emergency departments, ambulance and general practice.
For medical assistance contact:
Diver Emergency Service: 0800 4DES 111
First Aid for Diving Emergencies Flowchart
First Aid For Diving Emergencies.pdf
Diver Safety
Before diving, take a few minutes to review the safety training learned during SCUBA training courses.
This includes:
- Diving Equipment checks
- Emergency Equipment checks
- Emergency Procedures
Some areas to review are:
Predisposition to Decompression Illness (DCI)
- Fitness to dive
- Alcohol and / or lack of sleep
- Multiple ascents
- Multiple days diving
- 4 deep dives
- Diving at altitude
- Exertion during diving
- Cold water
- High CO2 levels
- Exercise after diving
- Hot showers after diving
- Flying or driving to altitude after diving
Avoiding DCI
- Appropriate training
- Avoid the previous list if you can
- Plan your diving day
- Revise computer use / backup tables
Planning a dive
- Depth
- Duration
- Surface intervals
- Decompression requirements and appropriate safety margins
- Current and state of tide
- Exit point
First Aid for DCI
- ABC - Airway; Breathing; Circulation
- Patient a. flat on back (conscious)
- b. Recovery position (unconscious).
- High flow oxygen 15 Lpm (Hudson mask does not provide 100%.)
- Call for assistance (DES) 0800 4 DES 111 or 09 445 8454, these are toll free. The Diver Emergency
- Service will advise you as to where and how to seek medical assistance.
- Consider risk of DCI in dive buddies if dive profile similar.
- Watch carefully. They can get worse!
Diving First Aid 10 Commandments
- Safety of Rescuer(s)
- Basic Life Support
- Posture
- Oxygen
- Rest and protect
- Observe and record
- Consult
- Specific Care
- Evacuate as indicated
- Secure diving equipment
Information for DES (0800 4DES 111 or 09 445 8454)
- Your name
- Name of the patient
- The telephone number you are at
- You will be asked to remain at that number until you are rung back by the duty diving doctor. (this should not be more than 5 mins)
Please bring to the hospital
- Any record of the diving, i.e., log book, dive recorder or computer. Include all diving within the previous seven days.
- Medical history and current medications
- Remember to secure any equipment used to aid in investigating the cause of the problem.
Evacuation
- There are few dive areas in the South Island from which road evacuation can be accomplished below 300 m.
- Road transport is adequate if quicker or nearly as quick as air transport.
- Keep patient below 300 m altitude or cabin pressure.
- Direct transfer from dive site to Christchurch Hospital is preferable if patient stable.
- Helicopter has limited range so will often transfer patient to fixed-wing via base hospital.
- For referrers, see Patient Referral and Transfer Procedures on CDHB Intranet, HealthPathways, Blue Book and provided to all Emergency Departments in our region.
Safe Diving!
What is Hyperbaric Oxygen Therapy (HBOT)?
 Hyperbaric oxygen therapy is the administration of oxygen at a higher than normal atmospheric pressure, that is used to treat a limited but diverse range of illnesses. It is the primary treatment for disorders such as decompression illness, arterial gas embolism and carbon-monoxide poisoning.
Hyperbaric oxygen therapy is the administration of oxygen at a higher than normal atmospheric pressure, that is used to treat a limited but diverse range of illnesses. It is the primary treatment for disorders such as decompression illness, arterial gas embolism and carbon-monoxide poisoning.
It is also an effective adjunct in a combined program involving dressing changes, surgery and antibiotics for the enhancement of healing in non-healing 'problem' wounds.
This includes:
- radiation tissue injury (both soft tissue and bone)
- selected problem wounds including diabetic ulcers
- chronic osteomyelitis
- crush injuries, and
- some skin grafts and flaps
How does Hyperbaric Oxygen Therapy work?
Hyperbaric oxygen therapy is the medical use of 100% oxygen at increased pressure. It works in a variety of ways in the body. This increased pressure provides more oxygen to the body than is possible under normal conditions. Most treatments are between two and three atmospheres of pressure, and the pressure change closely approximates scuba diving.
This increase of pressure drives more oxygen into body tissues and wounds that are lacking adequate levels of oxygen (called hypoxia) speeding wound healing and helping the return of normal tissue functions.
How often are Treatments Given?
The length and frequency of treatments is worked out for each person and the condition. Hyperbaric oxygen may be an important part of total care, including wound care, surgery and medication as indicated. For most patients, treatments are daily - Monday through Friday - and treatments may last 2 - 2 1/2 hours. Some emergency conditions will require only one or two treatments. In most cases of wound healing support, the effects are gradual, and 20 to 50 treatments may be required.
Who gives me my HBOT Treatments?
 Christchurch HMU has doctors who have had specialised hyperbaric medical training. The medical team includes anaesthetists and General Practitioners.
Christchurch HMU has doctors who have had specialised hyperbaric medical training. The medical team includes anaesthetists and General Practitioners.
While in the chamber, treatments are managed by either a Registered Nurse or Diving Medical Technician with specialised training in hyperbaric medicine. An attendant is always in the chamber throughout treatment. The treatment is managed outside the chamber by a technician trained in pressure chamber operations. Medical care is rapidly available during treatments.
What will I feel during the HBOT treatment?
 Everyone feels fullness in their ears as their eardrums adjust to the change in the chamber pressure. This is very similar to the feeling experienced when in an airplane or elevator. Instruction will be given on how to 'clear' ears, or equalize the pressure before treatment. If anyone experiences pain in their ears, the treatment is paused briefly until they are better.
Everyone feels fullness in their ears as their eardrums adjust to the change in the chamber pressure. This is very similar to the feeling experienced when in an airplane or elevator. Instruction will be given on how to 'clear' ears, or equalize the pressure before treatment. If anyone experiences pain in their ears, the treatment is paused briefly until they are better.
Once the treatment begins air hisses into the chamber and it gets warmer. This will return to normal once the treatment pressure is reached.
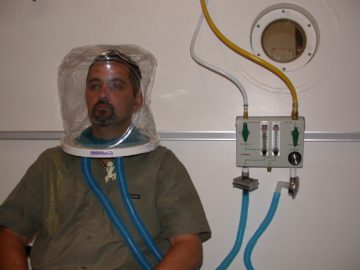
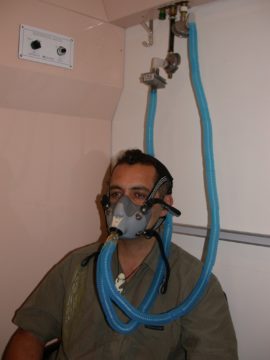
During the treatment patients breathe from a special oxygen circuit through either a close fitting face mask or a clear plastic head-hood.
The attendant is there to deal with any problems straight away.
What are the risks and benefits of HBOT?
Benefits
Depending upon the reason for coming to the Hyperbaric Medicine Unit, treatment can provide one or more of the following benefits:
- Increased oxygen delivered to injured tissue
- Greater blood vessel formation
- Enhanced wound healing
- Improved infection control
- Preservation of damaged tissue
- Elimination of toxic substances
- Reduced effects for toxic substances
- Reduction or elimination of tissue obstruction by gas bubbles
Risks
There are risks to HBOT, but most of them can be dramatically reduced with the proper management. The risks can be divided into two types, physical and safety risks.
Physical Risks
- Ear Discomfort
The increasing pressure in the hyperbaric chamber can cause ear discomfort and injury to eardrums. If unable to equalise the pressure by swallowing or yawning, a surgeon can make a small temporary hole in the eardrum, as used in children with 'glue ears'. This is called a myringotomy, and will heal quickly once treatments are finished. About 15% of patients have some degree of problem with clearing ears, this is usually only minor.
- Oxygen Toxicity
Oxygen toxicity can occur, affecting less than 1 person in 3,000-10,000, only once every few years in Christchurch. Signs of oxygen toxicity are tingling in the fingers, nausea, dry cough, chest pain and convulsions. Recovery is rapid and complete, although alarming when it happens.
- Visual Changes
During a long course of HBOT a reduction in visual acuity may be noticed. This is reversible in nearly all patients, returning to pre-treatment levels over several weeks or months. Sometimes this may interfere with such things as reading road signs from a distance, so extra care may need to be taken during the course of treatment.
- Other Physical risks
Other uncommon problems caused by the pressure change are pain in the sinuses or in teeth with poor fillings or cavities. On very rare occasions, damage to lungs may cause serious injury or death.
Safety Risks
Fire is a higher risk when the chamber is under pressure because of the increased level of oxygen in the hyperbaric chamber. All patients and staff remove all extra items that might be a hazard.
Items that cannot be taken into the chamber:
- cigarettes
- lighters
- matches
- excess paper (other than 1 reading item)
- newspaper
- jewellery/watches (other than diving watches)
- metal objects
- contact lenses
- hearing aids
- cell phones or any other battery operated device
- hand/pocket warmers and heat pads
Patients will be asked to remove anything with oil in it, such as:
- lipstick
- hair oil
- hair spray
- ointments
- linaments
- makeup
- cologne or perfume
Staff will arrange clothing to wear during the treatment. An undershirt of 100% cotton may be worn, to reduce the risk of electrostatic sparking.
Clothing not allowed in the chamber includes:
- wool, silk or synthetic textiles
- nylons
- polypropylene
What else do I need to know?
- For nearly all patients, treatment is painless and uneventful but takes up a lot of time and may get rather boring.
- No smoking 2 hours prior and 2 hours after treatment. Smoking decreases the amount of oxygen that can be transported by the blood. It is very strongly advised that patients do not smoke during the course of treatment as it reduces the likelihood of the HBOT working properly. Advice on smoking cessation is available from the nurses.
- People with diabetes on Insulin need to take their insulin and regular diet prior to treatment and, during the treatment, a suitable snack will be provided.
- Go to the toilet before the start of each treatment.
- Remove contact lenses and hearing aids before your treatment.
- Avoid fizzy drinks for 2 hours prior to your treatment.
- Ring the unit for any cancellations, but treatments should be daily.
- Get a flu vaccine and avoid people with coughs and colds during treatment. Getting a cold may make ear clearing difficult for a week or two.
If you have any questions or concerns, talk to your hyperbaric doctor or nurse.



