[Video length: 10:27 minutes]
[Music plays.]
[Title: Welcome to the Christchurch Oncology Service]
[Morgan Lambert, Radiation Therapist] Hi, my name is Morgan. Welcome to the Christchurch Oncology Service.
I’m one of the team of radiation therapists who will meet along your journey through our department.
By now you would have spoken to one of our radiation oncologists about receiving treatment for your cancer. The type of treatment that you will have depends on where we’re treating and the type of cancer that you have.
We hope to answer any questions that you may have during your time here and guide you through the process from planning all the way through to your actual treatment.
[Title: What to Expect]
[Dr Lisa Johansson, Radiation Oncologist] My name is Lisa Johansson. I’m a radiation oncologist here at Christchurch Public Hospital. I’d like to explain to you what you can expect when you come for your planning session and treatment.
Many patients are little frightened when they hear they need radiation treatment.
This is entirely natural and I think this is because you just don’t know what to expect.
During this presentation, we’ll follow a patient through their radiation treatment process so that you can understand what it involves.
Radiation therapy is a form of cancer treatment that can be given once a day, five days a week.
When radiation is delivered, you’ll not see or feel anything.
Radiation treatment is an important treatment option for cancer. In our department, we use modern and safe radiation treatment machines.
We aim to kill the cancer cells while keeping the radiation dose to the surrounding healthy cells as small as possible to minimise side effects.
The treatment staff are highly trained to make sure that your treatment is delivered safely and that you are kept as comfortable as possible during your treatment.
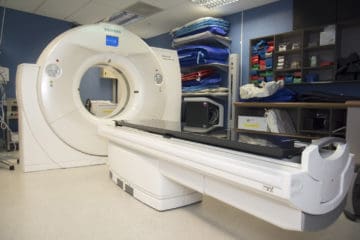
[Title: Planning CT Scan]
[Morgan Lambert, Radiation Therapist] When you arrive for your CT scan, please check in at reception. We’re you will be asked to take a seat in the main waiting room.
A radiation therapist will take you through to another room to discuss the process of the CT scan.
We’ll hope to answer any of your questions that you may have. And if you have any considerations or special needs that we need to know about, now is the time to let us know.
From there, we’ll take you through to scanning room. Firstly, with your permission, we’ll take a face photo with your hospital ID for identification purposes.
We’ll then get your positioned on the bed in the same position you’ll be for treatment every day.
We’ll help position you on the treatment table and ensure you’re as comfortable as possible. We have a number of positioning aids we can use to get you in the correct position for your treatment.
It’s important that you are as comfortable as possible as you’ll be in this position for treatment every day.
We do have to get to the skin in the area that we’re treating but we will ensure that we cover you up as much as possible.
Pen marks are then drawn on your skin with a marker. Sticky dots are placed over top of these, so the doctor can see on the scan where the pen marks are drawn.
The radiation therapists leave the room while the CT scan is being taken. We’re watching you the entire time. Remember to keep nice and still, breathe away normally.
The CT scan is very quick, only a minute or two and totally painless. You won’t see anything, or feel anything when the CT scan is being performed.
When the radiation therapists re-enter the room, keep still until we say otherwise.
We’ll take some photographs and measurements for verification purposes when you return for treatment. This information will go on your confidential hospital electronic record.
With your permission we’d like to do some small tattoo dots to help position you for treatment.
If you’re having treatment to head a neck area, a custom-made mask is used to keep your head still, this also means that marks can be drawn on your mask rather than on your skin for correct positioning.
We have two types of masks, the first for the head area, and the second is slightly longer for the header neck region.
Should you need a mask to be made, this will be done before your CT scanners performed.
With consultation with your radiation oncologist the best mask will be chosen for you. You can breathe, see, and hear through the mask comfortably. It’s made with thermoplastic material and heated in a warm water bath.
After a few minutes the mask becomes warm and soft, we then mould over your facial features to get a good fit. We cool it down using cold flannels and ice packs for it to set.
This can take anywhere from two to five minutes. The CT scan is then completed with your mask on.
[Title: Planning Your Treatment]
[Morgan Lambert, Radiation Therapist] When you’re planning CT is done, a team of radiation therapists along with your radiation oncologists will plan and customise your treatment for you.
Every patients treatment is unique. It is designed purely for you and your needs.
The radiation oncologist will decide on the area they want to treat and how much dose they want to give.
The radiation therapist will then work out the best plan for you. Depending on the complexity this may take from two hours, to several days to plan.
We design a plan to treat the area the radiation oncologist has outlined, while still reducing the dose to other organs and tissues as much as possible.
Once the plan is done, it undergoes a comprehensive quality assurance process to ensure it a safe and accurate for treatment.
What we have shown you up until now is what is needed in preparation for your radiation therapy treatment, which ideally will start in two to three weeks of your CT planning appointment. This depends on the type of cancer that you have, when you had surgery, and if you’re having any chemotherapy.
Next we’ll follow a patient through their treatment journey.
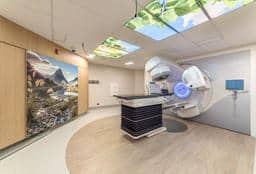
[Title: Radiation Treatment]
[Morgan Lambert, Radiation Therapist] On the first day of treatment check in with reception and take a seat in the main waiting room. From there, one of the radiation therapists will come and collect you for your treatment education session.
The radiation therapist will explain what to expect for treatment, will give you your appointments for the rest of the week, and we give you the appointments one week in advance. We’ll then take you through to get changed in preparation and you and the radiation therapist will go around to the treatment machine.
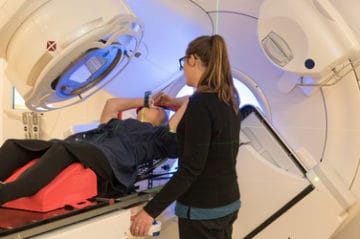
What we’d like to do now is get you set up in that same position you were for your CT scan. We work in the dark, so we’ll turn the lights down and we use laser lights from the walls to line you up to those tattoo dots or marks we gave you at CT.
Your job is just to lie there nice and relaxed, breathe away normally, and try not to help us when we move you. We load your details onto the computer and cross-check against your planned data.
Each appointment is approximately 10 to 20 minutes. Most of this time has spent setting you up in the exact same position you were for your CT scan. This time varies from patient to patient depending on what we’re treating.
You won’t see or feel anything when you’re on the bed. You’re just here buzzing noise when the machines turned on.
We usually have music to listen to during treatment, and you’re more than welcome to bring your own music along.
You’ll be in the room on your own when the radiation is on. We have cameras and microphones, so we can see you and hear you all times if you need us just call or wave out.
We may take an xray picture of the position that you’re lying in and we overlay this with your CT scan.
We’re then able to make any changes as necessary to get you in the correct position. The number of treatments may vary from one, to longer course over several weeks. If longer than a week, you’ll catch up with your radiation oncologist once a week.
After treatment, you won’t be radioactive. So you’re safe to interact with friends, family, pregnant woman, and children.
[Title: Radiation Therapy Side Effects]
[Dr Lisa Johansson, Radiation Oncologist] Sometimes during an after your radiation treatment, you may notice side effects. These side effects may include things like diarrhea, tiredness, hair loss, and nausea.
The side effects depend on the area that we are treating. For example, you won’t lose the hair on your head unless we are treating your head.
Not everyone gets the same side effects, many patients have no, or very minimal side effects.
Sometimes we use chemotherapy with your radiation treatment. If this is the case, we will coordinate your chemotherapy appointments with your radiation appointments.
It’s important to let us know how you are, so we can meet your needs while you’re in this department. You will see a radiation oncologist, or one of our registrars, once a week.
If you ever feel unwell, please let your treatment team know and they can get you to see the nurse or doctor as needed.
[Julia Bryson, Dietician] Our role down in the radiation department is to provide advice on dietary modifications, nutritional supplements and tube feeding for a lot of the cancer patients that require it.
It’s really important to try and maintain your weight during treatment, as this can help you recover faster from the effects of cancer, and effects of the radiation treatment. It’s important to try and continue to eat a variety of foods from all the food groups if you’re able to.
Some patients struggle with this, and if you’re unable to eat well due to decreased appetite, swallowing difficulties, or the treatment side effects, you might require nutritional supplements such as these, Ensure Plus, or Fortisip
The dietitians we’re available down in the radiation department and we can provide tailored nutrition advice depending on your situation.
[Morgan Lambert, Radiation Therapist] As well as the dietitian we have other services available to help and support you along your cancer journey including social workers, interpreters, and Māori health workers.
The Cancer Society also has an information centre located on the ground floor of the oncology department.
It provides information about radiation therapy, other services, and any other support that you may need during your journey.
We hope you know a bit more about what is involved when you come for your radiation planning and treatment. I hope we’ve answered some of the questions that you may have from the start.
We realise this is a whole new experience for you and your family, so any concerns that you may have please let us know we can help guide, support, and care for you along the journey with us.
[Credits: Canterbury District Health Board, proudly supported by DRY JULY.]